Myasthenia Medication Handout
Printable patient-friendly list of medications to avoid.
NeuroResidents
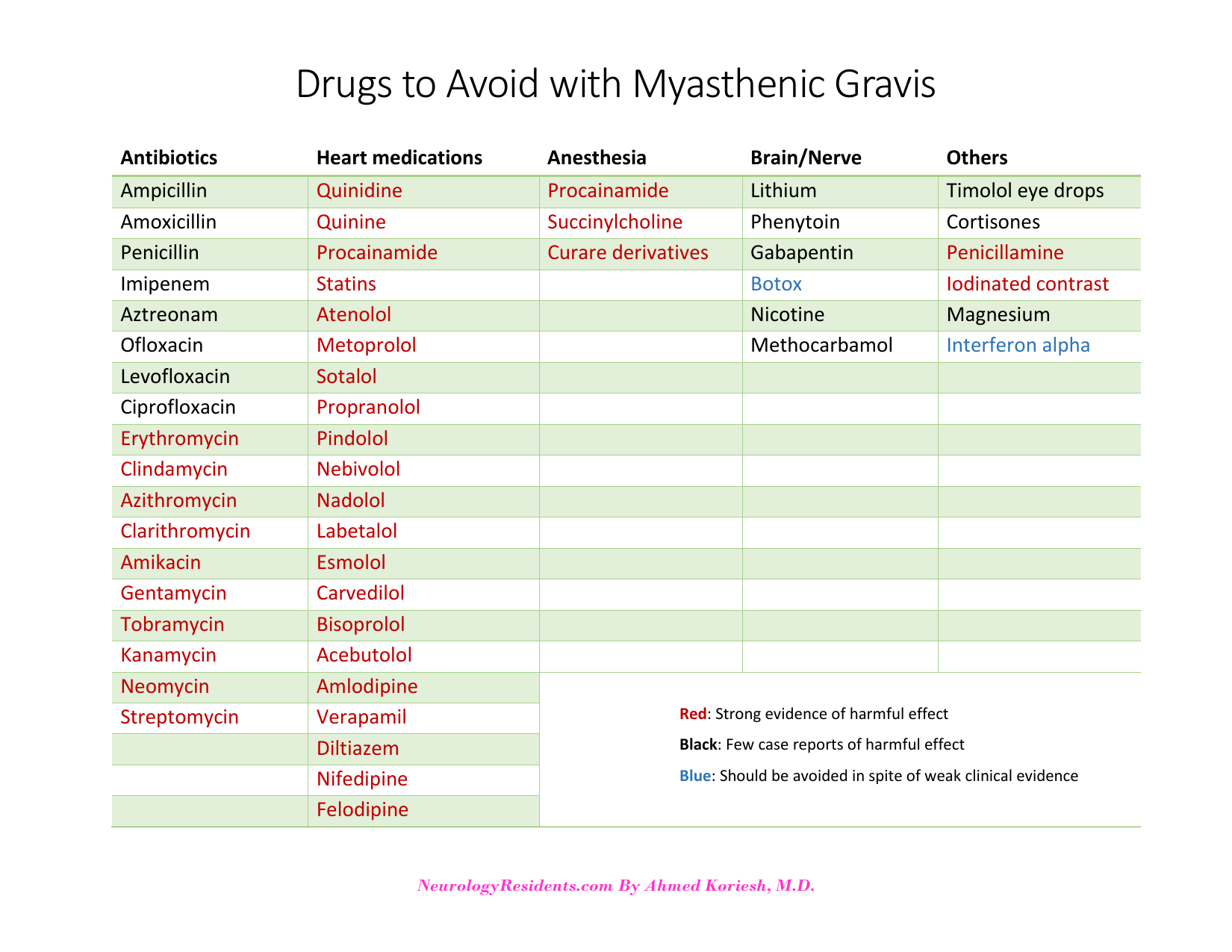
Antibiotics: Quinolones – Monobactams – Lactams – Macrolides – Aminoglycozides
Antiarrythmics: Quinine – Quinidine – Procainamide
BP medications: Beta blockers (including timolol eye drops) – Calcium channel blockers
CNS medications: Antiepileptic drugs – Lithium
Local anasthetics: Procainamide
Neuromuscular blocking agents: Succinylcholine – Curare medications
Others: Penicillamine – Steroids (needs supervision) – Iodinated contrast agents – Magnesium containing medications
..
– The 20/30/40 role: alarming values if FVC < 20ml/kg or NIF < 30cmH2O or MEP < 40cmH2O. These measures help to guide the level of admission (ICU/step down/floor), not to guide the decision for intubation. If FVC < 20ml/kg –> ICU admission is preferred.
– FVC is the most sensitive measure, NIF/MEP are effort dependent and less reproducible compared to FVC. Moreover NIF/MEP are unreliable if the face mask is leaking.
– Don’t depend on the numbers only for intubation. Patient should be either in respiratory distress while resting in bed without activity or hypercapnic to consider intubation.
– No respiratory distress –> no need for respiratory support –> admit to step down
– Mild/Moderate respiratroy distress –> consider BIPAP or Hiflow nasal cannula if BIPAP is contraindicated (secretions – nausea – vomiting). It must be done in ICU for lose monitoring of respiratory distress, if didn’t improve (RR decrease, less use of accessory muscles) –> intubate.
– Severe respiratory distress –> intubation and mechanical ventillation.
Use these templates as educational starting points. Adapt to the patient, the attending, and local policy. Do not place PHI into the public text editor or email workflow.